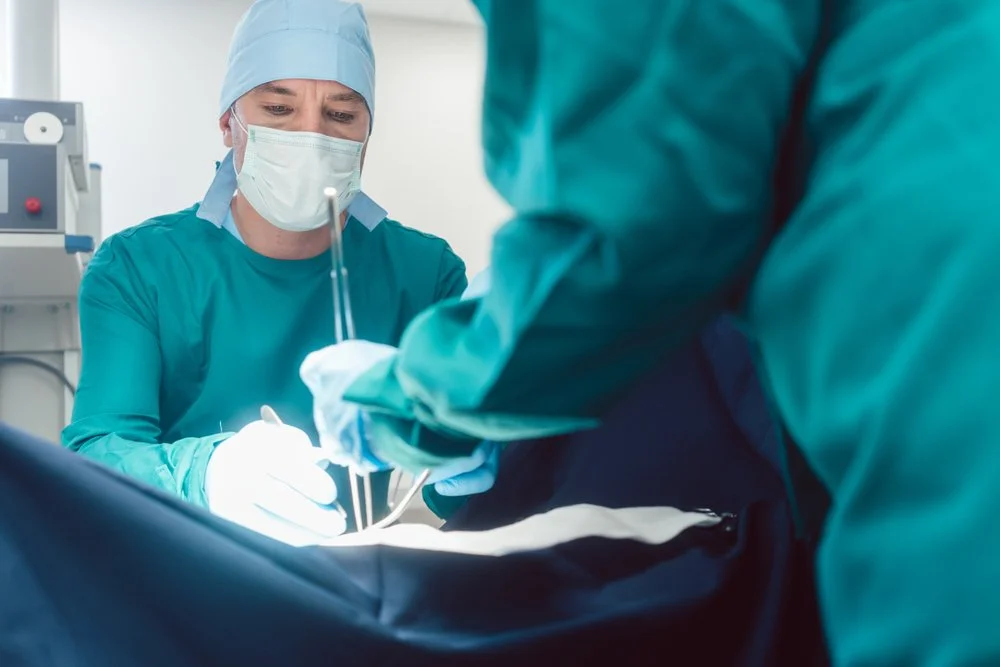
Emergency vs. Unplanned C-Sections Explained by a Midwife
When families hear the words “C-section,” a lot of assumptions come with it.
Many people don’t understand the causes of a Cesarean or what truly leads to one. There’s a lot of misunderstanding about obstetrical complications that do and do not lead to a Cesarean, things like a big baby, a cord around the neck, or a long labor. It’s true that those things can contribute to a Cesarean, but they usually don’t.
There are actually two very different categories of Cesarean birth: unplanned and emergency. Understanding the difference can change how you prepare for birth and how you process it if your plans shift.
In this article, we’ll explain the difference between unplanned C-sections and emergency C-sections, how they typically unfold, the emotions that follow, and what families deserve to know before decisions are made.
Key Takeaways:
Unplanned and emergency C-sections are not the same, the biggest difference is time.
Most Cesareans are unplanned, not true emergencies.
In many situations, there is time for questions and informed consent.
How decisions are communicated can shape how a birth is remembered.
A powerful birth is defined by agency, safety, and support, not delivery method.
First, What Is a Cesarean Birth?
A Cesarean birth is a surgical procedure in which a baby is born through an incision in the abdomen and uterus. In the United States, about one in three babies are born this way.
Some Cesareans are planned ahead of time for medical reasons. Others are not anticipated and become necessary during labor. And a small number are true emergencies that require immediate action.
What’s the Difference Between an Unplanned and an Emergency C-section?
While many people mistakenly think unplanned and emergency C-sections are the same thing, they aren’t.
What Is an Unplanned C-Section?
An unplanned Cesarean is what it sounds like: someone was planning a vaginal birth and, for one reason or another, needed, or chose, a Cesarean birth.
They are usually not done in a rush. A spinal or epidural is placed before the baby is born, and the partner or other parent can typically be in the room. The room is often calm, even if emotions are mixed.
Most unplanned Cesareans follow a pattern that unfolds over time. Labor may stall despite support and movement. The baby may show signs of tolerating labor less well over several hours. Or interventions like Pitocin may not produce the progress everyone hoped for. There is usually time for conversation, questions, and thoughtful consent.
Common reasons for an unplanned Cesarean include:
Labor that is not progressing despite adequate time and support
Gradual signs of fetal intolerance to labor, where the baby’s heart rate patterns suggest increasing stress
Maternal infection during labor
A fetal position that makes vaginal birth unlikely
With an unplanned C-section, there is usually time for conversation, questions, and thoughtful consent.
What Is an Emergency C-Section?
An emergency Cesarean is a true emergency. It usually needs to be completed within minutes of the decision being made.
In these cases, the baby is often born within 5 to 15 minutes. The birthing person may receive general anesthesia, which works more quickly than a spinal or epidural. Their partner may not be allowed in the room due to urgency and safety protocols.
Situations that can lead to a true emergency Cesarean include:
A sudden, severe drop in fetal heart tones that does not recover
Cord prolapse, when the umbilical cord slips ahead of the baby and becomes compressed
Significant maternal bleeding
Placental complications such as placental abruption, when the placenta separates from the uterus prematurely
These situations are rare, but when they happen, speed matters.
It’s important to understand that emergency Cesareans make up a small fraction of total Cesarean births. Most fall into the unplanned category, where there is at least some time to slow down and talk.
The Gray Area Between Emergency vs. Nonemergency C-Sections
In real life, C-sections do not always fit neatly into categories.
Sometimes there’s urgency, but not crisis. Heart tones are not awful and do not require general anesthesia, but they are not reassuring enough to keep waiting in the delivery room.
This is where communication matters most.
While this may be a routine workday for providers, it is a defining moment in a family’s life. How decisions are communicated can shape how the birth is remembered long after it’s over.
That’s why how decisions are made matters just as much as what decisions are made.
What Happens When Birth Plans Change?
It’s fairly common for birth plans to change. These changes can range from things like where you push or who catches your baby, to the mode of birth being different from what you imagined.
What makes the biggest difference is not that someone gets exactly the birth they planned for. Instead, it’s that they felt they were the ones making the decisions to respond to changing information without coercion, manipulation, or fear.
If someone is worried about their baby and decides to have a Cesarean for safety, they will often feel much more at peace with the decision than if they feel pressured and didn’t have time to ask questions or consider their options.
Regardless of how a birth unfolds, if someone feels that they were in the role of the executive, the one making decisions, they will feel more positively about it. That sense of agency makes all the difference when birthing plans change.
Related: How to Create an Effective Birth Plan with a Midwife
How We Talk About Urgency As Midwives Without Creating Fear
It’s quite rare that we go into the hospital from a planned home birth and go immediately to a Cesarean. Truly, there have only been a handful of those in our entire career.
What is more common is that someone is having a long labor, goes into the hospital for an epidural, has Pitocin, and after a period of time, the decision to have a Cesarean is reached because a vaginal birth seems unlikely.
We talk about the possibility of Cesarean birth with each client. We talk extensively about hospital transfer before a planned home birth to avoid surprises.
When we feel urgency about getting to the hospital, it does not always mean there will be a Cesarean. Often, a vaginal birth at the hospital can still happen even if something is no longer safe for a home birth.
For example, if fetal heart tones are concerning but stable, we may recommend transfer because we do not have access to a NICU team or advanced respiratory support at home. That baby will often still be born vaginally. The hospital simply has more tools available if needed.
This is an important distinction:
A transfer to the hospital does not equal a Cesarean. A moment of concern does not automatically mean surgery. Often, it simply means we are moving into a setting with more tools available, while continuing to aim for a safe vaginal birth.
When there is urgency, we speak honestly, frankly, and lovingly. Despite our orientation toward valuing natural birth and vaginal birth, there are clinical signs that demonstrate this may be one of those rare cases where a Cesarean is safest.
We explain what we’re seeing and our recommendation, and then we let the birthing parent make the decision. The trust that we cultivate is what makes that all possible.
Questions You Deserve to Ask Before a C-Section
Even in urgent moments, you still deserve information.
In most unplanned situations, there is time to ask:
What are the risks and benefits of a Cesarean in my specific case?
What are my options besides surgery?
What are the risks of waiting?
What challenges do you see with my Cesarean specifically?
What parts of my birth plan can we keep in the operating room?
Can we do immediate skin-to-skin?
Can I nurse in the OR or in recovery?
Can my partner, doula, or midwife be present?
Can we keep conversation in the room focused on my surgery and my baby?
Can I meet the surgeon who will be operating on me?
Asking these questions does not slow down necessary care. In most unplanned situations, there is time for them. When there truly is no time, your provider should be able to clearly explain why.
Remember, even in surgery, this is still your birth.
What Is the Role of a Midwife When a Surgical Birth Becomes Likely?
Our role shifts, but it doesn’t disappear.
If a C-section becomes necessary, we are there as advocates, liaisons, and helpers. When we are allowed in the OR, we help explain what’s happening. We support the other parent as they hold their baby. We advocate for skin-to-skin, early breastfeeding, and respectful communication.
Related: The Role of a Midwife in a Successful & Healthy Home Birth
What Are the Emotions That Follow a C-Section?
After a Cesarean birth, many families wrestle with questions.
If I had done something differently, would the outcome have changed?
Why me?
If there was a genuinely frightening moment, that fear can linger long after the birth is over.
There is often grief for the birth moment they imagined but did not get. Feeling their baby’s skin on theirs immediately. The uninterrupted first gaze. The embodied experience of pushing their baby into the world.
At the same time, there may be relief that everyone is safe.
Both can exist together.
As midwives, our role postpartum is to offer compassion, empathy, listening, processing, and honest answers. We help families integrate what happened so that it becomes part of their story without defining them.
What Makes a Birth Powerful Even When It Ends in an Unplanned C-Section?
In our eyes, a birth is powerful when someone feels they made the decision.
You can have a birth that looks completely different from what you imagined. But if you felt informed, respected, and free to choose without pressure, there is often peace that follows.
If someone felt pushed into something they did not understand or were not ready for, that is when trauma is more likely to take root.
A powerful birth is not defined by the delivery method, whether vaginal or surgical. It is defined by informed choice, support, and safety.
A Grounding Truth to Carry Into Labor
Cesarean births save lives.
Every birth has the potential to become a Cesarean birth because we do not control everything. We do not choose our baby’s position, how they tolerate labor, or whether unexpected complications arise.
Part of the courage of mothers is being open to the possibility of abdominal surgery as part of their birth story. Making peace with that possibility ahead of time can make it less overwhelming if it becomes necessary.
And at the same time, there are many, many things you can do to significantly lower your risk of a Cesarean.
Because preparation, trust, and continuous support matter.
And no matter how your baby is born, you deserve to feel informed, respected, and powerful in the process.
If you’re preparing for birth and want care that prioritizes informed choice, clear communication, and deep trust, we’d love to walk that road with you.
Schedule a consultation and let’s talk about the kind of support you want around you when it matters most.